This glimpse inside a 5-day-old zebrafish’s heart shows why they’re often used as a model organism in cardiac studies. The fish’s heart rate is similar to humans and its two-chamber heart — one atrium and one ventricle, both seen here — serves as a simplified version of ours. Check out the slowed-down section of the video to clearly see blood filling and expanding one chamber before it’s pumped onward. Perhaps the most unusual feature of the zebrafish’s heart is its ability to regenerate; after amputation of up to 20% of its ventricle, the fish can fully regenerate its heart. That’s a pretty incredible recovery, especially when you consider that the heart has to keep pumping the entire time! (Video credit: M. Weber/2023 Nikon Small World in Motion Competition)
Tag: heart

Flow in the Heart
Few flows are more integral to our well-being than blood flow through the heart. Over the course of our lives, our hearts develop from a few cells pushing viscous blood through tiny arteries to the muscular center of a vast circulatory network, capable of powering us through incredible physical feats. What’s most astonishing about all this is that the heart goes through all these changes and adaptations without ever pausing.
Peering into the heart to see it in action is difficult, but researchers today are combining imaging techniques like CT and MRI with computational fluid dynamics to build patient-specific heart models. Not only does this help us understand hearts in general; it’s paving the way toward predicting how a specific treatment may affect a patient. Imagine, for example, being able to simulate and compare different models of an artificial heart valve to see which will work best for a particular patient. We’re not to the point of doing so yet, but it’s a very real possibility in the future.
To see some examples of predicted and measured heart flows, check out this video by J. Lantz. In the meantime, happy Valentine’s Day! (Image credits: Linköping University Cardiovascular Magnetic Resonance Group, video source; via Another Fine Mesh)

Inside a Heart
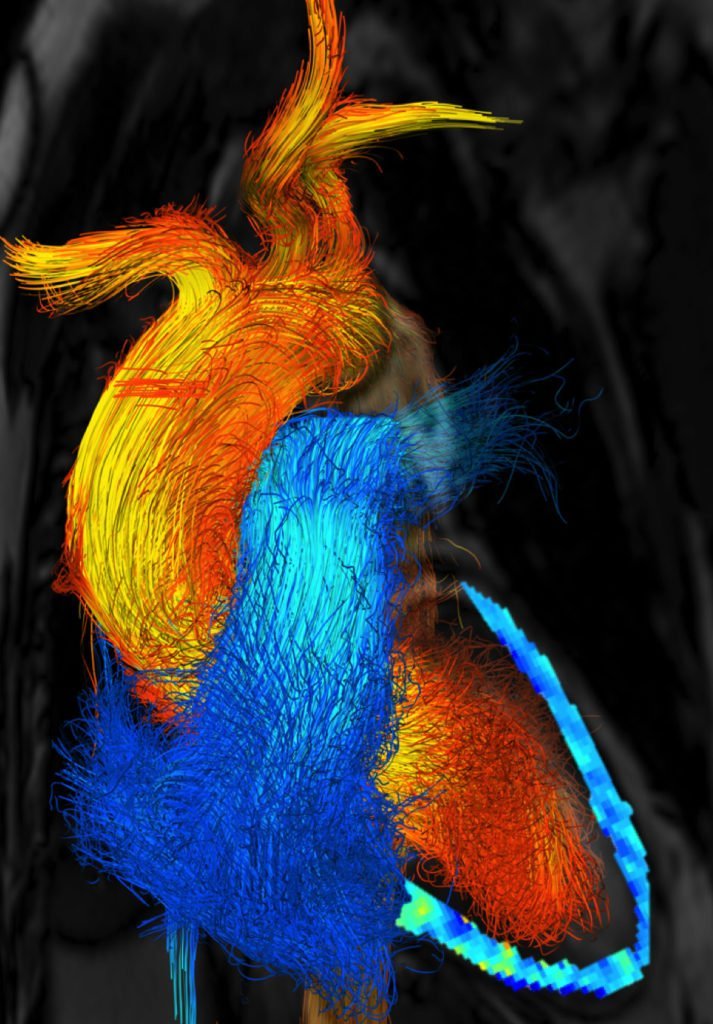
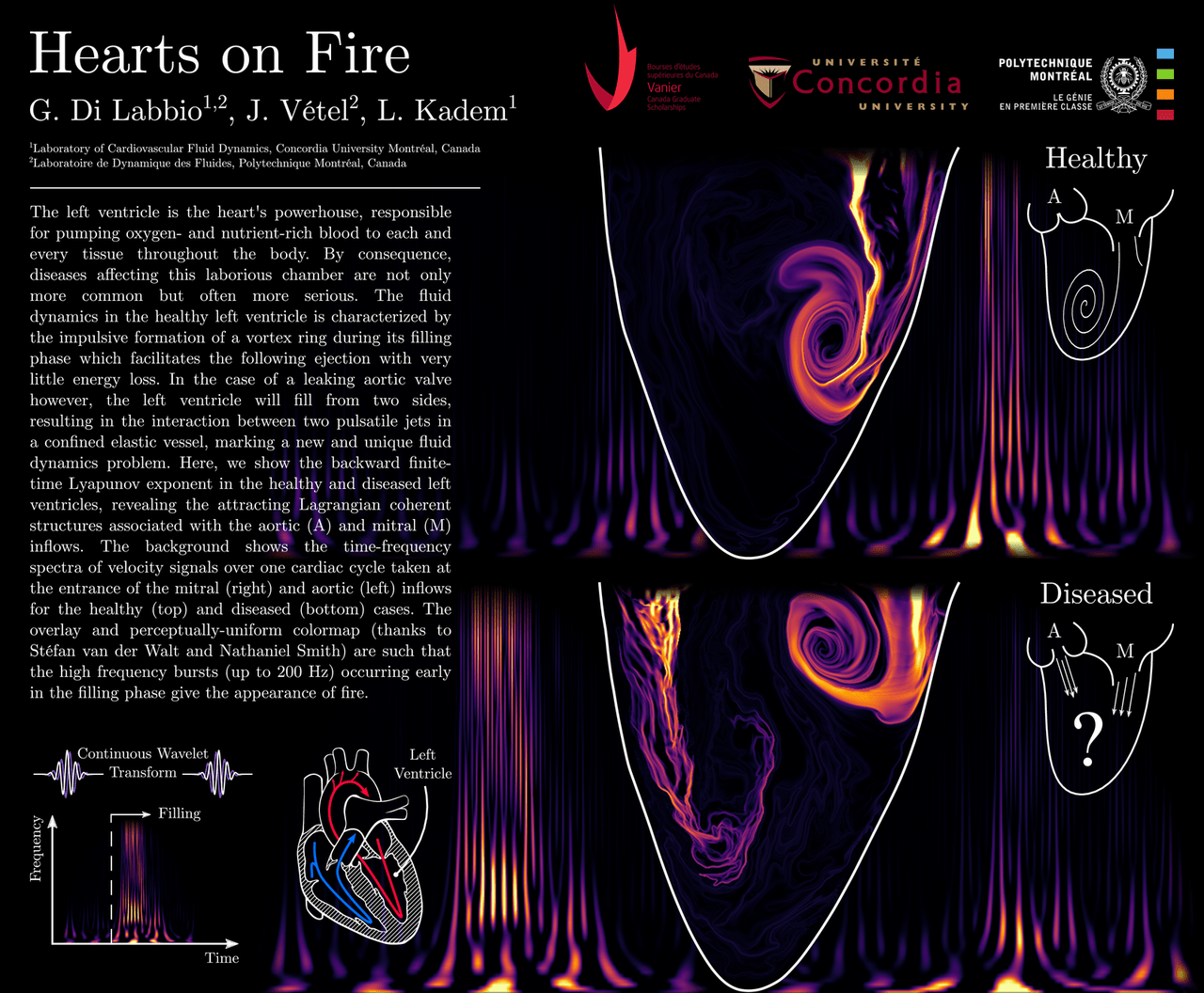
You may not give it much thought, but there is important fluid dynamics happening inside you every moment of every day, especially inside your heart. Of the four chambers of the heart, the left ventricle has the thickest walls, reflecting its important task: pumping oxygenated blood throughout the body. In a healthy heart (top of poster; click here for the full-size version), a vortex ring and trailing jet fill the ventricle when the mitral valve opens. Then the ventricle contracts and pumps blood out the aortic valve and into the rest of the body.
But for individuals with a leaking aortic valve (bottom of poster), things look different. Blood leaks back through the aortic valve at the same time that the mitral valve opens to allow freshly oxygenated blood back in. The two inflows disrupt mixing in the chamber, and, instead of pumping fully-oxygenated blood into the body, the left ventricle has to struggle to pump a less-oxygenated mixture into the body. (Image credit: G. Di Labbio et al.)
ETA: (Research paper: G. Di Labbio et al., arXiv)

Blood Flow Simulations
Though we may not often consider it, our bodies are full of fluid dynamics. Blood flow is a prime example, and, in this video, researchers describe their simulations of flow through the left side of the heart. Beginning with 3D medical imaging of a patient’s heart, they construct a computational domain – a meshed virtual heart that imitates the shape and movements of the real heart. Then, after solving the governing equations with an additional model for turbulence, the researchers can observe flow inside a beating heart. Each cycle consists of two phases. In the first, oxygenated blood fills the ventricle from the atrium. This injection of fresh blood generates a vortex ring. Near the end of this phase, the blood mixes strongly and appears to be mildly turbulent. In the second phase, the ventricle contracts, ejecting the blood out into the body and drawing freshly oxygenated blood into the atrium. (Video credit: C. Chnafa et al.)